latest
The government has performed a U-turn on compulsory vaccinations for NHS staff – but is it the right decision?
The government’s policy reversal will ease workforce pressures in the NHS and social care, but the problem has been caused by a long-term reluctance to address staff shortages
"Successive governments have had plenty of opportunity to address strategic workforce problems but have failed to do so. It has taken an emergency on the scale of a pandemic to force government to think about how to address staff shortages." Greg Allen, CEO, FCC
What does a fit for purpose health and care system could look like? There are probably so many different answers to that question – depending on who you ask.
One thing of which I am sure is that the foundations of such a system are built on the right values and also enough well-trained staff to deliver care and service. Whatever expectations people have of the health and social care system, without enough suitable staff in place to do the work, the service will not operate effectively.
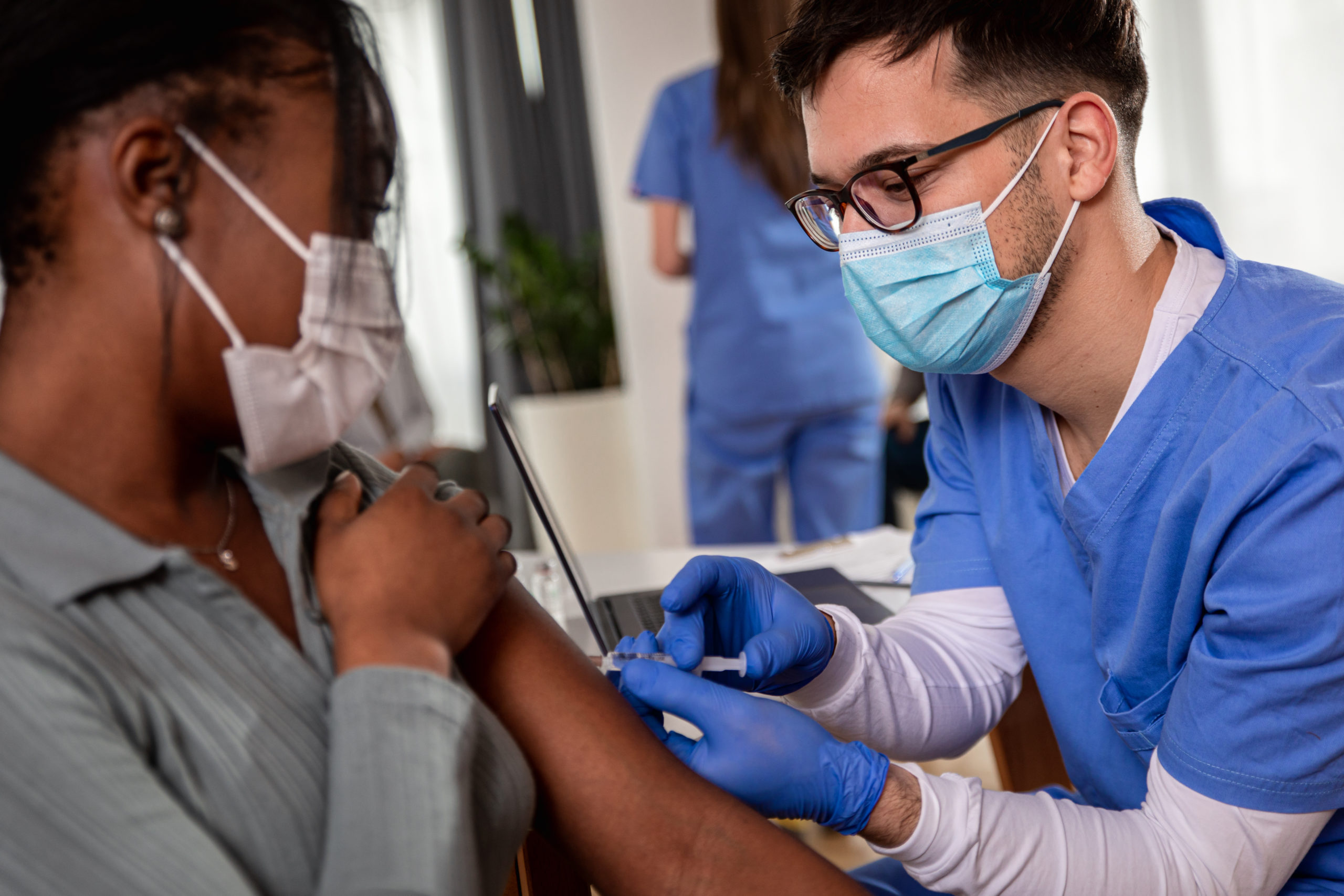
In this context, the issue of compulsory vaccinations for NHS and care sector workers has come to the fore. And now, we have heard that the government is to carry out a U-turn on its policy of compulsory vaccinations for these workers in England.
About 77,000 NHS workers have not yet received a single jab – that’s 5% of the total. The deadline for receiving jabs is 1 April. The policy was introduced because of fears that unvaccinated staff could put patients at risk.
‘Devastating’ impact on care
The compulsory vaccination policy was introduced first for care home staff (with a deadline given of 11 November last year), of whom 40,000 left frontline work rather than receive a vaccine. Nadra Ahmed, chairwoman of the National Care Association, says that the policy had a “devastating impact”.
So, is the government right to consider a U-turn? The decision has received a very mixed response. The BMA has welcomed it, while the chief executives of NHS Providers and the NHS Confederation have expressed concern about the message it sends about vaccination. NHS Employers have, understandably, expressed anger at the way the decision was communicated.
U-turns can be both helpful and unhelpful. There are good reasons for thinking this U-turn is the right thing to do. One is that the NHS in England currently has 100,000 vacancies: it can ill afford to lose another 77,000. A second is that Scotland, Wales and NI are not implementing a mandatory vaccination policy, meaning that NHS workers in England could easily seek work elsewhere if they lose their NHS job. Finally, the dominance of the Omicron variant suggests that the original Covid virus is mutating to be milder and less harmful.
A problem of the government’s own making
Up to a point, we can sympathise with the government’s position. While introducing mandatory vaccines might mean losing staff, not introducing them arguably puts the lives of vulnerable patients at risk.
But the way this U-turn has been handled as well as the wider workforce challenge are both problems largely of the government’s own making. We have seen growing and large numbers of staff exit the NHS in recent years. Successive governments have had plenty of opportunity to address strategic workforce problems but have failed to do so. It has taken an emergency on the scale of a pandemic to force government to think about how to address staff shortages.
The current strategic workforce issue was in the making ten years ago, if not before. Last year the Department of Health and Social Care ordered a review that looks at NHS workforce needs in the long term. The review is due to report this spring. In the meantime, we have an acute short-term workforce issue, highlighted by this government U-turn on its own compulsory vaccinations policy.
They say, “It ain’t what you do it’s the way that you do it.” In this case, it is about both what you do and how you do it. I am sure that the public’s expectations are that care and consideration for NHS and care staff is just as important as the care and service that they are expected to deliver, in ever-challenging circumstances.