latest
Patients at risk from virtual wards, clinicians warn
A plan to discharge 15% of Covid inpatients with pulse oximeters to ease pressure on hospitals is not supported by evidence, doctors say
“Virtual wards were necessary during earlier waves of the pandemic to manage covid-19 infection and reduce the pressure on hospitals. Such a model may be needed in the next few weeks given fears around the current wave of omicron, but the evidence on how effective they are for conditions beyond covid-19 is very limited.” Andrew Goddard, president, Royal College of Physicians
NHS England’s plans to expand the use of virtual wards for Covid patients has been criticised by the Society for Acute Medicine and the Royal College of Physicians, who fear that they could put patients at risk.
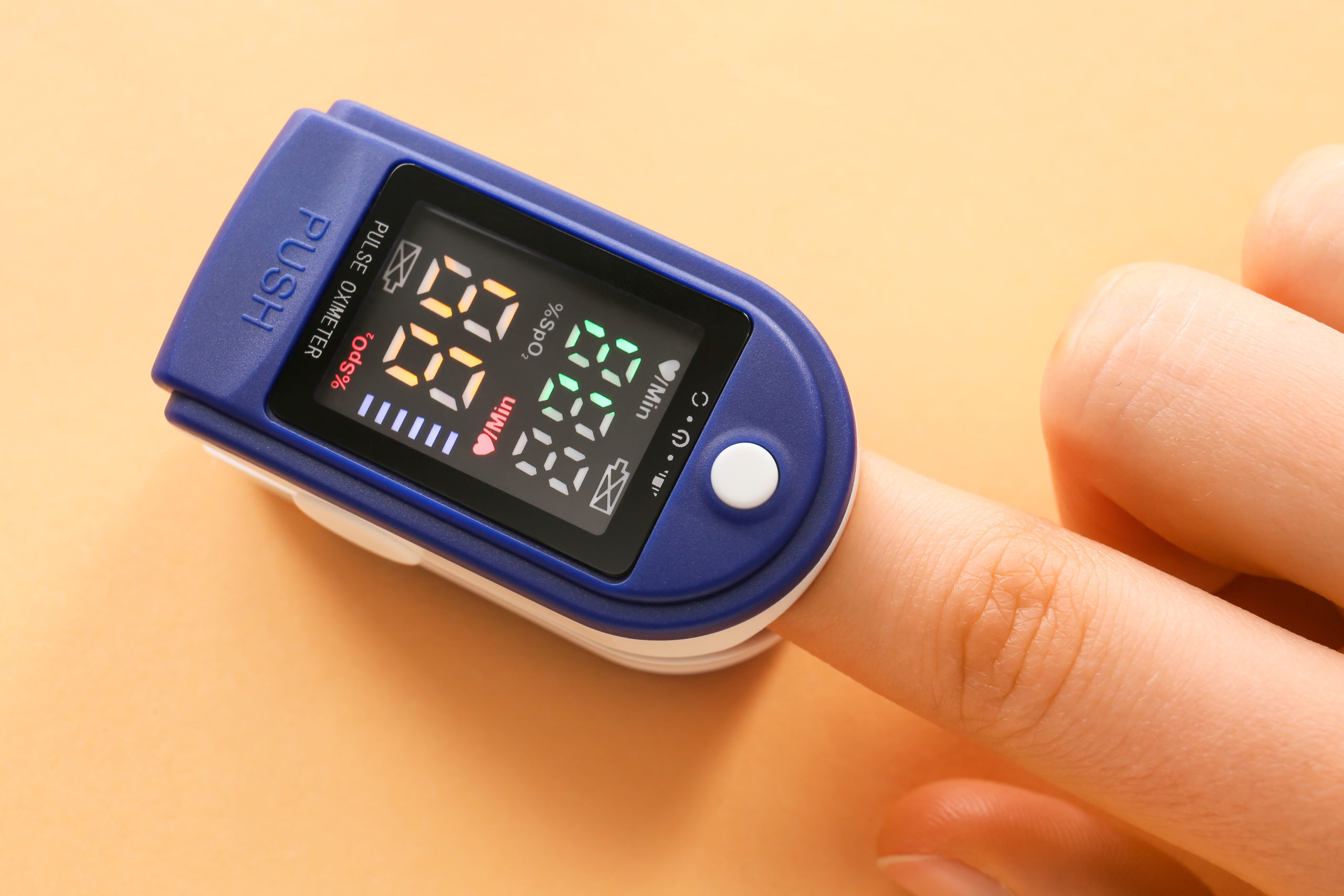
Under the virtual wards model, patients are discharged with pulse oximeters so that they can be remotely monitored. Just before Christmas, NHS England ordered trusts to make sure that 15% of hospital Covid patients are treated in virtual wards, in order to ease pressure on hospital wards. The longer-term aim is to extend the use of the virtual ward model to non-Covid patients.
At the time NHS England announced the plans, there were 7,000 Covid inpatients in English NHS hospitals, a figure that had risen to 16,000 by 5 January. If trusts carry out the plans, that will entail sending 2,400 patients home. HSJ reported that, even before the announcement, a number of trusts were planning to expand their virtual ward capacity, with one teaching trust looking to increase the number of patients in its virtual facility from 20 to 80.
Tim Cooksley, the president of the Society for Acute Medicine, told HSJ that while virtual wards had potential for the future, they “simply cannot be seen as a short-term mitigation measure which can be hastily rolled out mid-pandemic”.
The evidence base for the model proposed “remains light”, he said, adding: “In the short-term such projects will be resource-intense and during the midst of the pandemic that is going to be extremely problematic. The implementation of this requires careful clinical and operational management and it is vital that those with clinical expertise in the field, such as those working in acute medicine and primary care, are at the forefront of this work to ensure it delivers its potential impacts. It is also a long-term goal and that is how it must be treated.”
Evidence for effectiveness is limited
As well as expressing concern about patient safety, Cooksley said that the model could increase demands on staff: “Workforce pressures of virtual wards are likely to be significantly underestimated in what is already a depleted NHS workforce and this risks both the success of the implementation and, more importantly, patient safety.”
Andrew Goddard, president of the Royal College of Physicians, said there was not yet a strong evidence base for adopting virtual wards: “Virtual wards were necessary during earlier waves of the pandemic to manage covid-19 infection and reduce the pressure on hospitals. Such a model may be needed in the next few weeks given fears around the current wave of omicron, but the evidence on how effective they are for conditions beyond covid-19 is very limited.”
Similarly, David Oliver, a former president of the British Geriatrics Society and visiting fellow at the King’s Fund, told HSJ that the virtual wards model was “not a magic bullet” and it was too early to be attaching “ambitious national targets” to their use: “There are evaluations of virtual wards ongoing but [at present] we don’t have sufficient evidence to be setting targets of that level of ambition. Also, we can’t judge their success just by how many people are being managed outside hospital, because we need to look at their outcomes.”