latest
Getting Real: Don’t Push the Blame on Me
This month’s story “Don’t Push the Blame on Me” is the eagerly anticipated story from Anne Charnock, as a follow up to “All I Asked For”. The first part was a thought-provoking exploration of a controversial concept, which has stimulated a large amount of discussion and was recently shortlisted for the final of the British Science Fiction Association’s Short Story of the Year Award. Don’t Push the Blame on Me explores the lives of a family after they have experienced a “preemptive caesarean”, baby bag gestation and subsequent artificial birth. We experience a more detailed view of the wider healthcare system in place in the future context, seeing some of the long-term ramifications of the procedure described previously. In the first part of the story, the main character seemed reluctant to forgo a traditional birth and this proves to be a recurring theme at the heart of many subsequent concerns of Alice’s mother.
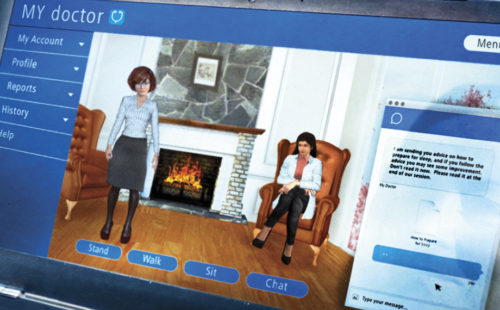
The selection of an avatar for this form of consultation is in some ways reminiscent of a form of experimental therapy being explored for the treatment of some symptoms of schizophrenia. AVATAR (Audio Visual Assisted Therapy Aid for Refractory auditory hallucinations) therapy for schizophrenia has been developed for those experiencing distressing auditory hallucinations (which not all people with schizophrenia experience). Through AVATAR therapy, people interact with an avatar representation of the voices they experience as part of their auditory hallucinations. A trained therapist then speaks to the individual through an on-screen avatar, using the words typically experienced during a hallucination. The person experiencing the therapy then confronts the avatar and the therapist concedes, becoming less hostile over the course of therapy. In a study published in 2017, AVATAR therapy was significantly more effective over 12 weeks for reducing the severity of auditory hallucinations when compared to controls engaging in supportive counselling. This approach to treating a complex psychiatric phenomenon is promising and certainly warrants further exploration as larger, long-term trials are needed to ensure safety and effectiveness for wider uptake. There are other researchers looking to adapt the therapy from on-screen therapy to a virtual reality (VR) headset, starting next month and concluding at the end of 2021. Later in the story, the main character is also offered VR content as a type of behavioural therapy, which has been trialed with some success for individuals living with anxiety. In a previous Getting Real post we explored VR content in more depth, including some of the pitfalls of highly personalized automatically generated content.
An intriguing feature of the consultation interface in this month’s story is the imitation of the main characters accent by the clinician avatar. Imitation is a behaviour which is exhibited by many species, in many instances for the purpose of learning motor skills. In humans, empathy and sharing of emotions appear to be a major component of imitation and mimicking behaviour. We copy movements, facial expressions, and vocal features to connect and better relate to our peers. In a previous blog, we covered the Echoborg installation, where a human actor is relaying the information from an AI system. In Don’t Push the Blame on Me it seems that this sort of interface may be in play in some scenarios and the main character is trying to work out if the first point of interaction is an AI system, an untrained human relaying information, or an inexperienced medical student rather than a fully trained clinician. A recurring theme of the Fictions series is the place of the human in a future underpinned by AI and an ongoing struggle related to purpose, fair treatment, and agency.
We are living through a pandemic which, alongside the immediate consequences of COVID-19, is causing delays in treatment and there are significant backlogs of non-COVID-19 cases to triage and assess. A recent report estimated that as of January 2021 there were 3 million fewer elective procedures performed and 22.1 million fewer outpatient attendances since the start of the COVID-19 pandemic. Some of these changes are a result of disruptions to clinical services and others have arisen from changes in patient behaviours. Telemedicine has helped connect patients and clinicians and will no doubt be useful going forward to help with the efficiency of service provision. There are many more disruptions on the horizon notably in relation to healthcare practitioners leaving, with one in four set to leave the service after the pandemic. There are serious concerns about the mental health of clinical and care personnel, fatigue and burnout are posing real problems for workers. Recently psychiatrists working with heath and social care professionals are calling for new care pathways specifically designed to support workers. The public health emergency is viewed very much from the perspective of COVID-19 cases. However, the longer-term recovery is as much about the prevalence of the virus as it is rebuilding a depleted and burnt-out workforce, triaging and treating a backlog of non-COVID-19 patients and either resuming or improving previous service provision. It is promising that applications for nursing courses are up on the previous year, however, there is still a huge workforce gap to be addressed.
It is interesting to consider which data are being used by the platform to triage and select appropriate care pathways. The stream of audio and video data are being analysed to detect key phrases and potential concerns to be followed up on for safety. Facial recognition technology (FRT) is not explicitly mentioned in the story but could be used in this context. FRT is considered controversial in many instances and has been trialed in a range of settings, including for policing and monitoring public spaces. Public attitudes towards FRT is at best skeptical and while such approaches have not entered mainstream medical practice, there are a range of approaches being developed for its use for diagnostic and treatment purposes. Indeed, there are also tools in development to improve communication and interaction for Telemedicine consultations, which have sparked recent controversies.
There were a range of other themes which would have been interesting to explore. Of particular interest is the link between the technology platform and an insurance-based healthcare model, this will no doubt be explored in another post before the series concludes in the summer.